
Critical Confusion Cascade: The Importance of Understanding and Implementing Guidelines for the Prevention and Management of Pain, Agitation/Sedation, Delirium, Immobility and Sleep Disruption (PADIS), in the Intensive Care Setting
by
Lori Mollmann, MBA, BSN, RN
(Sources for this article are included in the Sidebar.)
Introduction
Being a patient in the hospital, especially as a patient in an intensive care unit (ICU), can be extremely stressful for both the patient and the family. During their hospital stay, patients cope with several stress factors including:
- Pain, whether it is related to surgery or medical condition.
- Being away from their home and loved ones.
- Feelings of uncertainty and depression about their condition or prognosis.
- Disruption of routines.
- Sleep deprivation from staff interruptions and continuous monitors and alarm.
- Overall feeling of malaise and lack of energy.
In 2013, The Society of Critical Care Medicine developed guidelines for Pain, Agitation/Delirium, Immobility and Sleep Disruption referred to as PADIS (1). These issues are very common in the ICU population. General understanding of these guidelines is key to improving patient outcomes and patient experiences, as well as decreasing length of stay. The Society of Critical Care Medicine will be releasing revised PADIS guidelines this year, with the last revision occurring in 2018.

Pain
Pain is very subjective and can vary greatly between patients. Most pain is self-reported by the patient using a Numeric Severity Scale in which a patient reports pain between 0-10. In patients requiring mechanical ventilation, pain is generally reported/documented using the Critical Care Pain Observation Tool (CPOT) which involves observation of things such as guarding, grimacing, and/or being able to tolerate the ventilator, to comprise an overall pain score. In some cases, patients may have a history of chronic pain, or it may be post-surgical acute pain. Proper pain assessment can be further complicated by language barriers and cultural and religious beliefs. Methods for managing pain can include both pharmacologic and non-pharmacologic modalities. Traditional pharmacologic methods include intermittent intravenous push, oral administration, patient-controlled analgesia (PCA) or a continuous intravenous infusion. The most commonly used medications are morphine, hydromorphone (Dilaudid), fentanyl and oxycodone. Examples of non-pharmacologic modalities that are often used are cold compresses, warm packs, aromatherapy or soothing music. Proper attention to a patient’s vital signs and mentation are also integral parts of pain management strategies. Other components of PADIS, such as delirium and sleep disruption can occur if effective pain management is not achieved.
Agitation/Sedation
The incidence of agitation and anxiety in an ICU setting occurs anywhere from 50% to 70% either during admission or several days after admission (2). Factors that contribute to patient agitation include:
- Fear regarding critical illness or surgery.
- Financial and family worries.
- Unfamiliar surroundings.
- Pain and our unpleasant stimuli.
- Loud noises/alarms/bright lights.
Some of these concerns may be mitigated with proper assessment. This includes providing reassurance and answering questions regarding the environment, plan of care, or fears. If the agitation does not improve, the most common sedation modalities administered include Ativan, Versed, Valium (benzodiazepines) either oral or intravenous, as well as Precedex (alpha2-adrenergic agonist) and Propofol (non-barbiturate sedative) as a continuous infusion for short term sedation (3). While it is important to provide a patient with safety and comfort, if sedation is necessary, careful attention must be paid to the level of sedation. The most frequently used assessment tool for sedation is the Richmond Agitation Sedation Scale (RASS). The RASS scale consists of a 10-point scale that ranges from a +4 combative, violent, danger to staff, to -5 Unarousable, no response to voice or physical stimulation (4). Most sedation orders are written to titrate sedation to reach a RASS score of -2 Light sedation; briefly awakens to voice with eye opening for less than 10 seconds, as it is critical not to under sedate or over sedate a patient.
Delirium
Delirium continues to be a common occurrence among the ICU population, especially in older adults (6). Delirium is associated with prolonged hospital stays, increased mortality, increased cost of healthcare and a decrease in functional independence. According to the National Institute of Health (NIH), delirium occurs in roughly 20-50% of ICU patients who are not receiving mechanical ventilation and 50-80% of ICU patients requiring mechanical ventilation (5). Delirium assessment can be further complicated by baseline cognitive issues such as dementia. When assessing delirium, the most widely used assessment tool is the Confusion Assessment Method (CAM). The CAM was initially designed to assist non-psychiatric medical professionals to diagnose delirium (6). The CAM algorithm consists of four main areas for identifying delirium (6):
- Acute and Onset Fluctuating Course.
- Inattention.
- Disorganized Thinking.
- Altered Level of Consciousness.
With continued focus on properly assessing delirium, the CAM has proven beneficial to identify delirium in an inpatient setting (6). The CAM has become the most universal delirium assessment tool in part for ease of use and rate of accuracy (6). Sleep deprivation and delirium are intertwined. It is critical to conduct frequent assessments and it may be necessary to redirect and/or reorient a patient and provide patient centered care. Proper attention should be paid to avoid napping throughout the day and making sure lights remain on during daylight hours and encourage regular sleep/wake cycles.
Immobility
Early mobility in the ICU population is a vital part of recovery. Potential risks of delayed immobility include (7):
- Weakness
- Muscle Atrophy
- Pressure Ulcers
- Ventilator Associated Pneumonia (VAP)
- Deep Vein Thrombosis (DVT)
This lack of mobility can also intensify anxiety and depression. It has been found that early mobilization can reduce these risks to improve patient outcomes and decrease the length of stay (5). Strict adherence to early mobilization protocols is a must, along with working collaboratively with ancillary teams, i.e. Physical Therapy and Occupational Therapy, to achieve optimal results and decrease recovery time. If a patient is unable to ambulate, range of motion protocols should be utilized (7).
Sleep Disruption
Sleep disruption can significantly impact the recovery of critically ill patients and has been linked to short and long-term repercussions (8). These repercussions are represented in the Critical Illness and Sleep graph and include (9):
- Cognitive problems/Delirium
- Emotional Distress
- Immune System Compromise
- Mobility Issues
- Respiratory Compromise
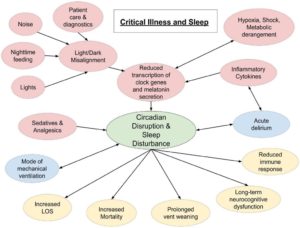
Several strategies can be implemented to limit disruptions to sleep including (8):
- Noise Reduction, Light Reduction, Sleeping Masks
- Alarm Volume Management
- Coordinating Care to Limit/Minimize Disruption
Barriers and Challenges
Barriers exist among critical care nurses concerning the use of the PADIS assessment tool. These barriers include (10):
- Knowledge Gaps
- Nursing Beliefs Concerning Patient Centered Care
- Resistance to Change
- Difficulty Coordinating Care with Multidisciplinary Team
- Lack of Time/Resources/Equipment for Training
- Managing and Monitoring all Aspects of PADIS
A study consisting of 112 ICU nurses illustrated that PADIS education programs were very beneficial in boosting nurses’ knowledge, skills and attitudes (10). Continuous efforts to achieve competency with using PADIS is pivotal for improving patient outcomes in an ICU setting.
Conclusion
The utilization of recommended PADIS guidelines in an ICU setting may reduce length of stay, reduce mortality, decrease days on mechanical ventilation and improve patient outcomes (6). It is essential that inpatient ICUs work toward providing formal standardized training and implementation to improve utilization of PADIS.
(Sources for this article are included in the Side Bar.)
Author: Lori Mollmann, MBA, BSN, RN
Greater Orlando AALNC Chapter, Director at Large
Owner: Mollmann Medical Consulting
Email: Lmollmann@att.net
Contact: 617-899-8463
_________________________________________________________________________________
CHAPTER MEMBER HIGHLIGHT
JILL CAMPBELL, BSN, RN, CPTC

Jill is an LNC and the owner of Campbell Clinical consultants, LLC. As a registered nurse for over 20 years, she has spent most of her career in the area of organ donation and solid organ transplantation. She also has experience in critical and perioperative care. Jill has a bachelor’s degree in nursing and completed a Legal Nurse certificate program through Florida Atlantic University. She has been a Certified Procurement Transplant Coordinator (CPTC) since 2012, and has served on multiple committees for the United Network for Organ Sharing (UNOS) and contributed to published works on organ allocation. During her career as a lead coordinator for the largest transplant organization in the US, she honed her expertise in organ donation, procurement, and transplant. She was involved at a national level in policy development, standards of care, and quality measures. This prompted her interest in legal cases involving proper consent of organ donors, equity in organ allocation, and protecting the rights of transplant recipients and donor families. In 2024, Jill established her legal nurse consulting company, in which she uses her experience to provide meticulous discovery within medical records, facilitate collaboration between healthcare and legal experts, and optimize the overall efficiency of legal proceeding in intricate medical cases. Jill’s primary home is near the beaches of Jacksonville, Florida, and she also has a residence in Atlanta Georgia. When she is not working on building her business, you can find Jill at a baseball game, walking on the beach, or hiking with her dog. Jill has been a member of AALNC since 2022, and the Greater Orlando Chapter of AALNC since 2023. In January 2025, she was installed as a Director at Large for the Chapter.
_______________________________________________________________________________

THANK YOU, JOAN MAGNUSSON!
On March 29, 2025, we celebrated our Chapter’s 35th Anniversary with a party/social at Seasons 52 in beautiful Altamonte Springs, FL! We had 25 members and guests present, and ate, laughed and networked for four hours! We were HONORED to have Joan Magnusson present! Joan was the first President of the Greater Orlando Chapter in 1990! Her support and mentorship of Greater Orlando Chapter members, has touched more lives and jumpstarted more LNC careers than any of us can count! We will FOREVER be grateful to her! (Some pics from the event.)

CONNECT WITH US
Connect with us on LinkedIn
Check us out at: https://orlandoaalnc.org
Contact us at: info@orlandoaalnc.org
Resources for Critical Confusion Cascade PADIS:
2. Pain, agitation and delirium in the intensive care unit – ScienceDirect
3. RxList – The Internet Drug Index for prescription drug information, interactions, and side effects
4. Richmond Agitation-Sedation Scale (RASS) – Physiopedia
6. The Confusion Assessment Method (CAM): A Systematic Review of Current Usage – PMC
9. Frontiers | Sleep and critical illness: a review
10. Clinical Impact of the Implementation Strategies Used to Apply the 2013 Pain, Agitation/Sedation, Delirium or 2018 Pain, Agitation/Sedation, Delirium, Immobility, Sleep Disruption Guideline Recommendations: A Systematic Review and Meta-Analysis – PMC
__________________________________

“SAVE THE DATES”
Be sure to watch for our publication, “SAVE THE DATES.” This publication includes LNC education programs offered by AALNC, and ALL of the AALNC Chapters! We are so excited for this joint Chapter activity! Watch for the next edition, coming to your inbox soon! And, don’t forget to check out the AALNC Event Calendar. It is filling up fast with 2025 events and programs! And mark your calendars for the Greater Orlando Chapter Update and CE Webinar Dates for 2025:
- NO CHAPTER MEETING IN APRIL – JOIN AALNC VIRTUAL FORUM 2025!
- May 20, 2025
- June 17, 2025
- July 2025 – SUMMER BREAK
- August 19, 2025
- September 16, 2025
- October 21, 2025, and
- November 18, 2025
Don’t forget our On-Demand Webinars. We have 19 On-Demand Webinars which are free for Chapter members and only $20 for non-Chapter members.
And check out the education programs from our fellow AALNC Chapters:
- Bay Area Chapter of Northern California at: https://www.bacnc.org/
- New Jersey Chapter at: https://aalncnjchapter.clubexpress.com/
- Pittsburgh Chapter at: https://aalncpittsburgh.org/
- Tampa Bay Chapter at: https://www.aalnctampa.com/
- Pacific Northwest Chapter at: https://www.pnw-aalnc.com/
CONTINUING EDUCATION INFO
The Greater Orlando Chapter of AALNC is an approved provider of Nursing CE through the Florida Board of Nursing and CE Broker, and approved by the following States: Arkansas, District of Columbia, Florida, Georgia, Kansas, Kentucky, Mississippi, New Mexico, South Carolina and West Virginia. We report CE directly to CE Broker in these states. For attendees from other States, we provide required documents for self-reporting CE to State Boards of Nursing.
LNC LAUNCHPAD – Q&A with Greater Orlando Chapter LNCs

In 2021 we started a new program for members, which we call “LNC Launchpad – Q&A with Greater Orlando Chapter LNCs.” This is a 1.5 hour session to provide guidance, answer questions, and suggestions. We limit the event to 10 participants, so we can mentor each attendee – whether new to the LNC practice or experienced and ready for a change – we are there for you! We have the 2025 dates selected so plan ahead, the slots fill up fast! (Registration for the May 2025 session will open mid-April, 2025.)
- May 6, 2025
- September 9, 2025
- November 4, 2025

LNC PROFESSIONAL DEVELOPMENT
AALNC and the Chapters are THE GO TO sources for networking and professional development in the field of legal nurse consulting. Want to learn of career opportunities? Want to stay up to date with the LNC industry trends? Want to hone your LNC skills and learn new ones? Then go to AALNC at https://aalnc.org and join now! Then go to https://orlandoaalnc.org and join our Chapter! And you can join ALL of the AALNC Chapters – for unlimited networking and LNC education!
WE ARE NEAR YOU! Maybe not geographically, but through your computer or phone. The Greater Orlando Chapter has members in 37 States and Canada! SINCE 2014, The Greater Orlando Chapter’s live Chapter Meetings with CE Programs have been broadcast virtually! So members and guests have been attending from all over the Country since then! Because of COVID, since 2020 all of our CE Programs have been virtual only. And though our Chapter Update Meetings and CE Programs are virtual, we are planning a Chapter Social early 2025, and we hope our members from all over the Country will find their way to Florida for some warm, sunny weather and a lot of LNC networking!
Greater Orlando Chapter Membership cycle goes from May to May of each year, with membership renewal being May 31. With this cycle, members who joined in 2024, membership renewal will be May 31, 2025.
If You Have Questions, Contact Us:
Email us at: info@orlandoaalnc.org
Or visit us at: https://orlandoaalnc.org
MEET THE 2025 GREATER ORLANDO CHAPTER OFFICERS
AND DIRECTORS

President: Robin Axtell, BSN, RN, LNCC
President Elect: Michelle Gaines, MNA, RN, CRNA
Immediate Past President: Tory Palivoda, BS, RN, LNCC
Secretary: Patty Mitchell, BSN, RN, CLNC
Treasurer: Jillian Talento, BSN, RN, CEN, LNCC
DAL: Pamela Borello, BSN, RN, CNOR, CNAMB, CSSM(e)
DAL: Jill Campbell, BSN, RN, CPTC
DAL: Christine Dorman, DNP, APRN, ACNP-BC, CCRN
DAL: Jenelle Lea, MBA, BSN, RN, CEN, GFN-C
DAL: Lori Mollmann, MBA, BSN, RN

